Testing for HIV at home: How Ottawa is piloting self-testing

Pictured, from left to right: Megan Francoeur, Kim McDermid, Patrick O’Byrne, Sarah Lachance, Marie-Odile Grayson, Lauren Orser
To end the HIV epidemic in Canada, it is important for people who are HIV-positive to know their status and to be linked to care. To do that, we have to reach people who are not testing now and make the process easier for them.
Self-testing in Canada
One promising initiative is HIV self-testing: a new technology that allows people to test themselves at home or with the support of a community health partner. Self-testing may make it easier for people who live far away from testing sites or whose responsibilities mean they can’t get to the sites when they are open. It may also help overcome the fear of stigma associated with going for testing.
While Health Canada has not yet approved HIV self-testing, there is a growing interest in its potential – particularly during the current novel coronavirus disease (COVID-19) pandemic, which has reinforced the need for different ways to deliver healthcare services, including sexual health services.
When Health Canada does approve the test (which we expect to be coming soon), it will be important to know how best to distribute the test and help people who receive a reactive test result to link to confirmatory testing, treatment and ongoing care. That research is now underway.
Introducing the GetaKit project
The GetaKit project launched on July 20, 2020, in the Ottawa region. People in Ottawa are now able to go to the GetaKit website, see if they are eligible to participate in the study, register, complete a baseline survey and order up to three free HIV self-test kits. The kits, which provide detailed, step-by-step instructions on how to take the test, are delivered to participants’ homes.
GetaKit uses a status-neutral approach: all participants are connected to support regardless of their test results. People who test negative receive post-test counselling and information on effective ways to protect their health, such as pre-exposure prophylaxis (PrEP). People who receive a reactive test result will be immediately linked to confirmatory testing and care.
Led by Patrick O’Byrne from the University of Ottawa (School of Nursing) and Ottawa Public Health, in partnership with the AIDS Committee of Ottawa, MAX Ottawa, and the Ontario HIV Treatment Network (OHTN), the GetaKit project will assess the feasibility and acceptability of a mail-out self-testing kit, as well as its impact on testing rates, HIV diagnoses and the ability to link participants with a reactive test result to care. The hope is that GetaKit will reach people at risk of HIV who have never been tested or have not tested for some time.
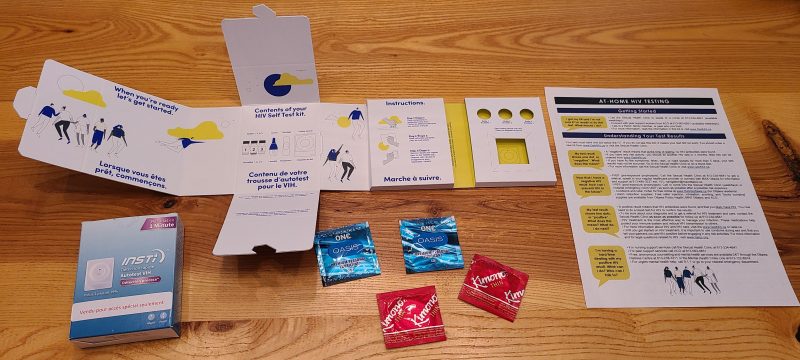
What’s in the kit?
The GetaKit packages are designed to be discreet to ensure the confidentiality and privacy of participants. Each HIV self-testing kit comes complete with:
- An INSTI rapid HIV test, produced by bioLytical Laboratories
- An expandable work station which clearly outlines the testing steps
- Linkage to care details, showcasing the partnerships and supports available in Ottawa
- Prevention materials (condoms and lubricant)
- Instructions in both English and French
Scale-up and self-testing expansion
The strength of GetaKit is its flexibility and scalability. Because people connect with the project online, it is easy to add and update content and to adapt information to different target populations and locations. The process of reaching people, sending out kits and connecting people to care, maps onto existing promotional platforms, distribution processes, linkage-to-care pathways and resources. The website and app make it easy to reach out to and communicate with participants for follow-up, and self-test kits can be utilized within organizations to facilitate supervised testing and linkage to care. The GetaKit project can also be combined with existing services such as harm reduction, PrEP and mental health services.
Self-testing does not replace point-of-care testing or other testing programs, but it may provide a highly effective way to increase access to testing. As self-testing programs expand, it is important for health organizations to examine the strength of their existing linkage-to-care pathways. What work is currently being done to discuss testing and risk and how can self-testing be utilized to strengthen that work? What can we do to increase testing rates, while ensuring that patients are not lost to follow-up care? These questions and more will help us develop effective self-testing services that can be scaled up and expanded across Canada.
Alexandra Musten is the senior lead of Testing & Clinical Initiatives at the Ontario HIV Treatment Network (OHTN). Her passion for testing was inspired while coordinating the monthly calls with the incredible and tireless members of the National Point-of-Care Testing Working Group. Please e-mail if you have any questions: amusten@ohtn.on.ca or getakit@ottawa.ca.