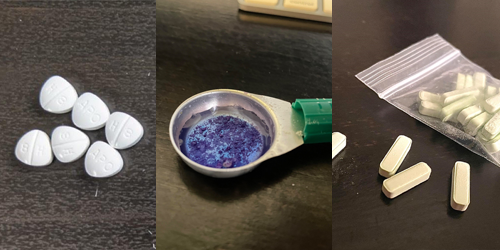
Splitting and sharing at overdose prevention and supervised consumption sites: What we learned
July 29, 2021 • By Nick Pineau, Sandra Ka Hon Chu, Corey Ranger, Matthew Bonn and Natasha TouesnardIn 2020, Health Canada started to hold consultation meetings with key stakeholders to review federal regulations governing overdose prevention sites (OPS) and supervised consumption sites (SCS). While multiple recommendations and suggestions were brought forward, one that was repeatedly identified by people who use drugs and other stakeholders as being of top concern was the inability to split and share drugs within OPS/SCS settings.